Zero.
That was the number of diabetes-related amputations recorded among intensive management patients in a recent report analyzing the impact of MLK Community Healthcare’s (MLKCH’s) Diabetes Management Center of Excellence program.
A new four-year analysis of results from the new Diabetes Management Center of Excellence, independently reviewed by the UCLA Center for Health Policy Research, shows that coordinated and comprehensive diabetes care can significantly improve outcomes. By the program’s fourth year, amputations among intensive management patients had fallen to zero. That stands in sharp contrast to a rate of 494 per 100,000 residents across the SPA 6 region.
Just a few years ago, diabetic amputation was the most commonly performed surgeries at MLKCH—reflecting the heavy burden of diabetes in South Los Angeles, where the condition is 37% more prevalent than in Los Angeles County overall. That is why we built our diabetes program: we wanted to address the barriers that make diabetes harder to manage.
The Diabetes Management Center of Excellence at MLKCH, launched in 2021 with lead support from the Good Hope Medical Foundation and matching support from the Rose Hills Foundation, operates as a comprehensive, evidence-based program incorporating American Diabetes Association clinical guidelines.
“In communities like South LA, the burden of diabetes is shaped not only by personal health behaviors, but also by access,” said Dr. Jorge Reyno, SVP of Population Health at MLKCH and co-author of the report. “Timely access to primary and specialty care, as well as medication support, education and consistent follow-up all play a critical role in helping people manage a chronic condition like diabetes before it becomes a crisis.”
All MLK Community Medical Group patients diagnosed with diabetes are enrolled in the program’s coordinated care model that includes medication management, preventive screenings and educational resources. High-risk patients (those with Type 1 diabetes, gestational diabetes or A1c levels greater than 9.0%) are enrolled in the Intensive Management Program to receive comprehensive management through a dedicated multidisciplinary team.
Instead of asking patients to navigate a fragmented healthcare system on their own, the program coordinates services around each patient’s needs.
Support includes a multidisciplinary care team—primary care physician, an endocrinologist, clinical pharmacist, care coordinators, case managers, a diabetes nurse specialist and community health workers—along with community programs such as Recipe for Health, ManUp! and Know Your Basics and technology tools including telehealth and BlueDrop remote monitoring to identify early signs of foot ulcers.
The analysis also showed strong improvements across several key measures:
- By the program’s fourth year, patients in the intensive management program reached 81% blood sugar control and 71% blood pressure control.
- Patient engagement improved as well. Appointment compliance reached 84%, up from a 50% baseline before the program began—showing that patients were not only enrolling in care, but staying connected to it over time.
- For patients enrolled at least nine months, blood sugar and blood pressure control rose to 85% and 74%, outperforming both national Medicaid and LA Care benchmarks.
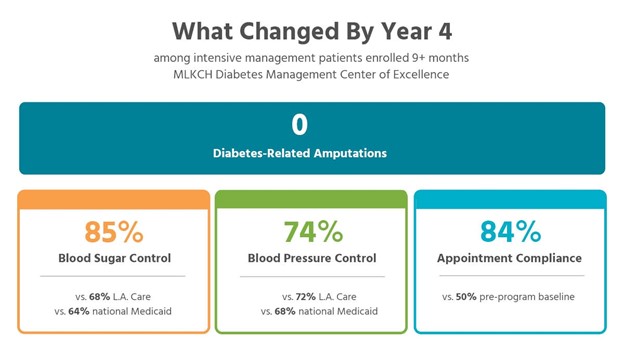
Encouragingly, the program showed steady improvement across all major indicators of diabetes care, with especially strong acceleration in Year 4. This sustained improvement suggests the program is reducing the barriers that have long made positive outcomes an elusive goal for patients in South LA.
In this case, the clearest sign of those improved outcomes among those with the greatest risk is simple: zero amputations.