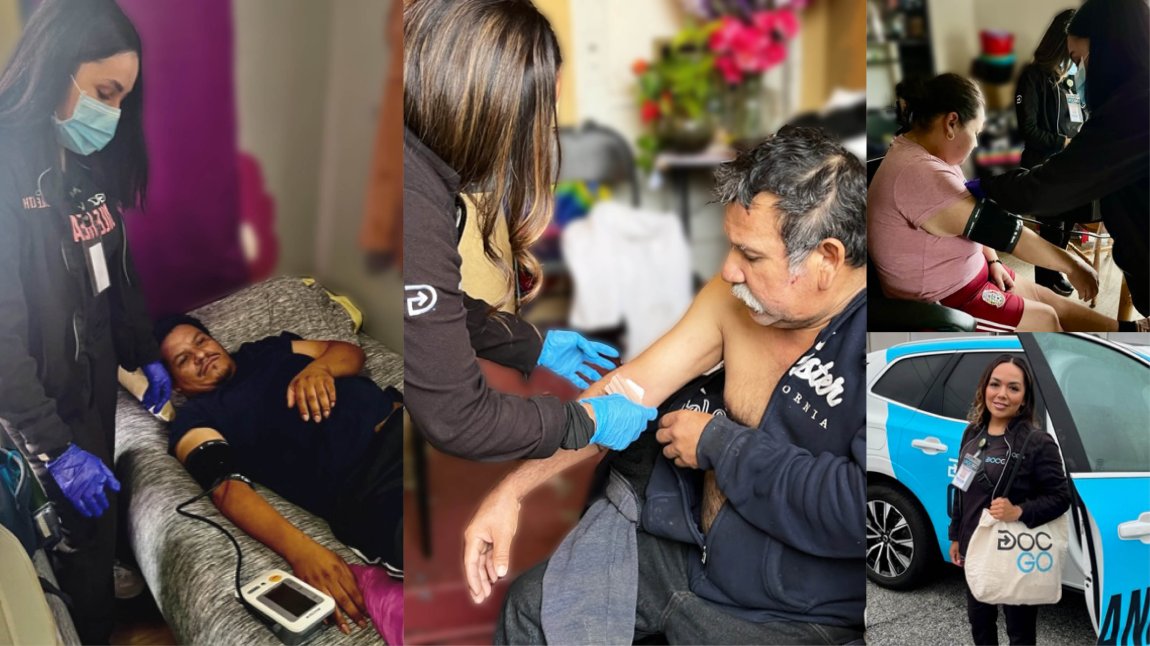
In a community with a severe lack of access to care, MLKCH’s Home Paramedicine Program brings the doctor to the patient
It has been four days since Josue Lopez Mendoza, 34, was discharged from MLK Community Hospital where he was treated for a serious abscess in his rectal area. Still in discomfort, he is pleased to greet nurse Michelle Robinson, when she visits him at the small, gated home in South LA where he lives with several family members.
This is the second time Robinson has stopped at this narrow street half a block from the roar of Interstate 110. She has been sent by the MLKCH Home Paramedicine Program, a mobile service that brings healthcare into homes across a vulnerable South LA community that often struggles to access care.
Indeed, home paramedicine, referred to as “house calls” in another era, is a response by MLKCH to the needs of patients as they recover from hospitalization—and an antidote to the severe doctor shortage in South LA’s low-income, majority-minority community. At last measure, the hospital’s service area lacked 1,500 doctors relative to communities of similar size in California.