Lung disease. Heart disease. HIV. Depression. Anxiety.
It’s just an average Wednesday for Orngiel Corbin.
As she waits for her cardiologist to arrive at an exam room at one of MLK Community Healthcare’s outpatient practice sites, Orngiel complains of lightheadedness, stomach upset, anxiety and more. She fingers the portable oxygen pump she takes everywhere and complains that the hot weather is making it more difficult to breathe.
It’s a lot to handle for anyone. Each condition that the 58-year-old resident of South LA suffers from requires one or more medications—a total of 20 in all each day. Orngiel’s treatments require regular doctor’s appointments, home monitoring and more.
On their own, patients with complex conditions like Orngiel are almost always overwhelmed. Remembering to take medication (often several times a day), find and travel to medical specialists, and not lapse into paralyzing depression that could put a stop to recovery, are just some of the challenges.
Fortunately, Orngiel has something in her corner that few vulnerable patients have: a coordinated team of experts, all under one roof, united by the desire to improve her health. In Orngiel’s case, this includes a primary care provider, a cardiologist for her congestive heart failure, a pulmonologist for her emphysema, an infectious disease doctor to manage HIV, an addiction medicine psychiatrist to help her fight a debilitating relationship with cigarettes and alcohol, and a therapist to support her on her healthcare journey.
“If I didn’t have this care team, I’d be dead,” she says simply.
Whole person care
Integrated care is something that all patients need but – especially in underserved areas like South LA—rarely get. A study in the International Journal of Integrated Care noted that the US has historically lagged in efforts to integrate health and social care compared to other high-income countries resulting in “remarkably poor” outcomes for patients. Yet research shows that patients who receive care not just for their primary diagnosis but for other health conditions that may impede their recovery are much less likely to be hospitalized.
It’s why MLKCH has received combined support of more than $1.5 million from Cedars-Sinai and the California Community Foundation to make integrated behavioral health care a routine part of regular, physical health care. That support has reaped big results; this August, MLKCH received a prestigious three-year accreditation from the National Committee for Quality Assurance (NCQA) for its efforts to ensure that patients in the underserved community of South Los Angeles receive high-quality, coordinated care.
Although Orngiel mourns her former vigor—the South LA resident once loved to camp, snowboard and boat—there is no question that MLKCH’s integrated approach is helping prevent a more precipitous decline.
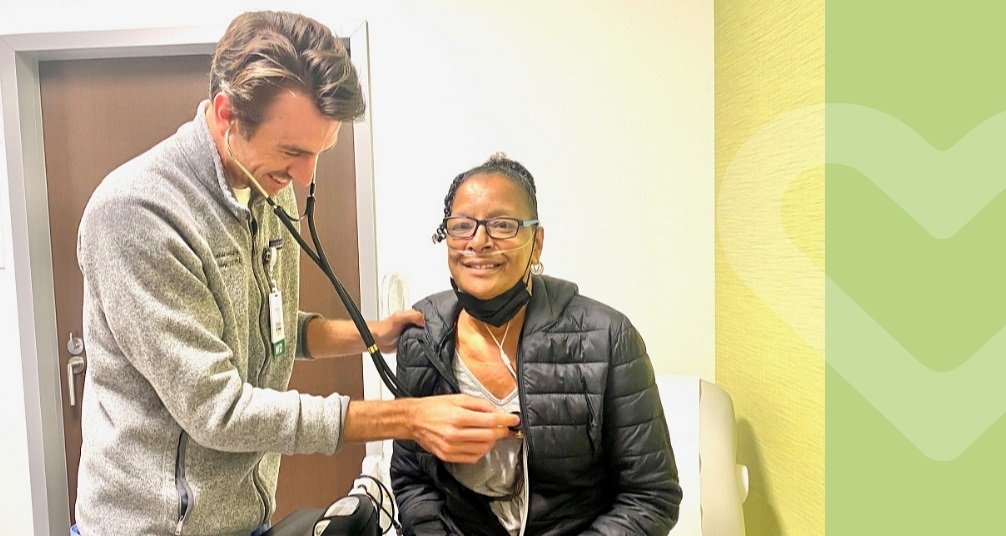
On a recent Wednesday at MLKCH’s Wilmington Clinic, two different members of Orngiel’s care team—Dr. James Pinney (a cardiologist) and Dr. Maita Kuvhenguhwa (an infectious disease doctor) have good news to report. Orngiel’s blood pressure, cholesterol, and T-cell numbers are good. Her kidney function is “better than it has been in many, many months,” according to Kuvhenguhwa. The heart monitor that Pinney gave her to wear at home to check for any dangerous arrhythmia found nothing unusual. “That’s good news,” says Pinney, who now doesn’t have to see her for another six months.
Her progress is only possible because all her doctors sit in the same office, share the same instantly-available electronic health information and can consult a colleague who may be sitting just steps away.
“A team approach seems obvious,” says Pinney. “But it’s actually less common that you’d think. A lot of patients in other health systems have to go one place for primary care, another for specialty care and yet another for tests and medications. When you’re low-income and may not have a car and you feel crummy, this can become a huge obstacle to progress.”